 Hot topic
Hot topicBelow is one of our selection of Hot Topics, important issues which sometimes generate heated debate over the facts or their interpretation. Click the GO button or the Blue title to trigger a customised search for relevant documents. Links to other documents. Hover over for notes. Click to highlight passage referred to. Unfold extra text

Copy title and link
| Comment/query | Other hot topics | Tweet
‘Hot topics’ offer background and analysis on important issues which sometimes generate heated debate. National programmes distributing the opiate overdose antidote naloxone have become the great hope for curbing the rise in overdose deaths, but England is lagging behind the rest of the UK – and planning for the likelihood not of recovery but relapse may for some services and patients be hard to accept.
Every nation in the United Kingdom saw increased drug misuse deaths between 2013 or 2014 and 2015. In raw numbers, in proportion to the general population, and probably too in proportion to the number of problem drug users, the increases ended at record levels.

Despite some complications, the consistent picture is that totalled across the UK deaths related to drug misuse rose steeply between 2012 and 2015, driven by a corresponding rise in deaths involving opiate-type drugs, and in particular, heroin ![]() chart right. Drug misuse deaths registered in the year increased by 68% between 2000 and 2015, and those involving opioids by almost exactly the same proportion, rising to 2,683 or 81% of the total. Public Health England’s 2015 report to the European drug misuse agency says 88% of drug poisoning deaths which actually happened in 2013 involved opioids, a proportion which has remained broadly similar since 2004.
chart right. Drug misuse deaths registered in the year increased by 68% between 2000 and 2015, and those involving opioids by almost exactly the same proportion, rising to 2,683 or 81% of the total. Public Health England’s 2015 report to the European drug misuse agency says 88% of drug poisoning deaths which actually happened in 2013 involved opioids, a proportion which has remained broadly similar since 2004.
What caused the upturns was a major talking point in 2016. Especially in England, commentators targeted the UK government’s recovery agenda for failing to maintain harm-reduction services and a harm-reduction ethos. Others emphasised the ageing of the heroin-using population as fewer young people join their ranks, leaving the overall population increasingly dominated by older and more multiply ill and vulnerable users who started using decades ago, a trend only briefly interrupted by the ‘heroin drought’ of (roughly) 2010 to 2012. Investment in treatment in England and national naloxone programmes in Scotland, Wales and Northern Ireland, did not prevent the upturns, but almost certainly moderated their steepness.
Whatever the causes, in terms of remedies the figures set the stage for naloxone – an antidote which specifically targets overdoses involving opiate-type drugs – to become the main new hope for curbing the rise in drug overdose deaths. Further forefronting naloxone is the 2016 revision to the Public Health Outcomes Framework for England – indicators of the nation’s health by which local areas are held to account. A sign of national concern, the revision added the rate of drug misuse deaths per million of an area’s population to the indicators. According to the Department of Health, it was a response to “a rising trend in drug related deaths over the last few years”. One relatively inexpensive way to directly target drug misuse deaths is for local areas to mount naloxone distribution campaigns.
While this hot topic focuses on naloxone, another has explored the overdose figures and overdose prevention though means other than naloxone programmes. To help absorb the messages, most sections below start with one or two introductory paragraphs which convey the essence of what follows. These paragraphs end in ![]()
![]()
![]() more ...
more ...
National naloxone programmes across the UK – but not in England
Naloxone is a drug which rapidly reverses the effects of opiate-type drugs, including the respiratory depression which causes overdose. It became the main new hope for curbing the death rate after in 2005 UK law was amended to permit emergency administration by any member of the public. The drugs naloxone reverses are not the sole cause of overdose deaths – benzodiazepines and alcohol play a big role – but across the UK, 88% of drug poisoning deaths in 2013 involved opiate-type drugs. Naloxone distribution has been aided by a medically approved kit and a relaxation of prescription-only requirements. Of all the UK nations, England has yet to take advantage of these developments to mount a coordinated national programme, but has contributed to the UK research base helping to validate naloxone programmes ![]()
![]()
![]() more ....
more ....
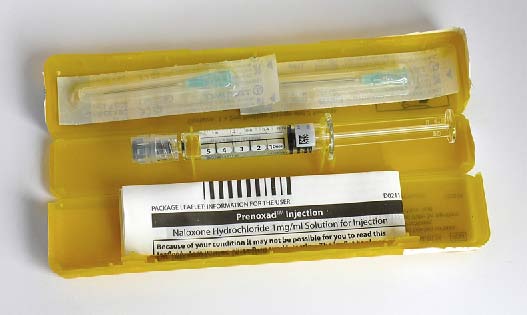
One of the types of naloxone kits approved for use in the UK
In May 2013 the naloxone ‘kit’ Prenoxad became approved in the UK for use in opioid overdose emergencies by non-medical personnel. The kit includes a pre-filled syringe, product instructions, and relevant first aid guidelines. Other kits have also been approved for general use. Approval was seen as an important step to widening availability. It meant GPs could prescribe kits to suitably trained drug users and with their permission to their associates and families. Patient group directions also enable doctors to authorise pharmacists and nurses to supply the kits.
Creating an exception to the need for a prescription, from October 2015 drug services in England and Wales were permitted without prescription to order supplies of naloxone and distribute these to drug users at risk of overdose or to people likely to be in contact with them, such as families, carers or hostel staff. Apart from this important exception, naloxone supply remains restricted by the prescription-only status which in 2012 the UK’s Advisory Council on the Misuse of Drugs wanted reviewed, after concluding that wider provision of naloxone could result in a reduction in drug-related deaths in the UK. In 2016 the Council acknowledged that so long as the only preparation approved in the UK is injectable, over-the-counter sales are unlikely to be allowed, but might be permitted for a version sprayed up the nose. Whatever it takes, the Council’s view was that widespread, easy and inexpensive access to naloxone is an important overdose prevention tactic.
Though more might be done in other UK nations, England has felt the brunt of criticism for not grabbing the opportunity offered by naloxone to reduce the death rate. Unlike other UK nations, in the name of localism England has so far not established a centrally driven national programme, a point made in a parliamentary question backed by 21 MPs tabled at the end of October 2014. Some local administrations are attempting to make naloxone available to all at-risk individuals, but from one such area came criticism that “coverage across England remains sparse”. Towards the end of 2014, the relative inaction in England and the recent increase in deaths there prompted the formation of the Naloxone Action Group “to push the agenda”.
Institutions in England can, however, take credit for grabbing the opportunity to validate naloxone through research in the UK context. The first large-scale UK follow-up study of naloxone-based overdose prevention training took place in England, and the results were published in 2008. It found these programmes can successfully be delivered to drug users in treatment, resulting in substantially improved knowledge and competence. Though only a few times, naloxone was used to save lives even within the study’s three-month follow-up period. The first UK randomised trial also ended up being conducted in England. The aim was to test prison-release naloxone by randomly allocating prisoners with a history of heroin use to be supplied a naloxone kit before release, versus a similar package not containing a naloxone kit. The researchers realised this methodology was inappropriate when they discovered that released prisoners were three times more likely to use their kit to save someone else rather than use it or have it used to save them. This meant it was unrealistic to expect the overdose death rate to be significantly lower among prisoners given the kits. Nevertheless, the trial produced evidence that lives might have been saved by issuing the kits. Of 112 prisoners who completed follow-up surveys when reimprisoned within six months, 21% said they had administered naloxone to themselves or another person before the arrival of a doctor or ambulance, versus just 9% of prisoners not issued kits.
While this and other evaluations of naloxone kit distribution programmes focus on how often the naloxone was used, the associated training gives trainees the skills and information they need to save lives without naloxone, a frequent occurrence which alleviates one of the main limitations of the schemes – kits not being available at the time and place of an overdose. In these situations, naloxone programmes may still have helped save lives, even though no administration of the drug has been recorded.
Evaluations of national UK programmes
Its record in reducing opioid overdose deaths shortly after release from prison is evidence of the effectiveness of Scotland’s naloxone programme, but one yet to be matched by evidence of effectiveness in other circumstances. Especially since the upturns in during-year drug misuse deaths in 2014 and those registered in 2015, it is unclear too whether Wales’s national naloxone programme has helped reduce deaths. However, naloxone kits have been used many hundreds of times. Together with training thousands of drug users and their contacts in other lifesaving techniques, it seems inconceivable that lives have not been saved, even if this is difficult to prove to scientific standards ![]()
![]()
![]() more ...
more ...
Scotland
Launched in 2011, Scotland’s national naloxone programme has been gathering pace, outside prison distributing 6,498 ‘take home’ naloxone kits in 2014/15 compared to 5,395 the year before, 3,132 in 2012/13, and 2,743 in 2011/12. In 2014/15 another 878 kits were issued to drug users leaving prison, down from a peak of 1,077 the year before. Reasons given for trainees being given a replacement kit indicated that in 2014/15 kits issued outside prison had been used 644 times, up from 424 times the year before and 212 and 132 in the first two years of the programme. An unknown extra number will have been used without the carrier returning for another kit.
An extremely high-risk period for former opiate users, in Scotland the proportion of opioid-related deaths occurring within four weeks of release from prison had been identified as the key indicator of success of a programme which had specifically and systematically targeted prisons. This was made the main metric in a study which compared opioid-related death rates in the five years before the programme’s implementation (2006–10) with those during its first three years (2011–13). A secondary indicator of success added in the proportion which occurred during the corresponding period after discharge from hospital, another high-risk period.

As the number of naloxone kits issued in prison increased, post-prison deaths accounted for a diminishing % of all opioid-related deaths in Scotland.
The post-prison period accounted for 9.8% of opioid-related deaths before the programme but 6.3% after – a 36% reduction taken as indicative of a lifesaving impact ![]() chart. Also reduced was the combined total of post-prison and post-hospital deaths as a proportion of the total. Routinely collected statistics indicated that the trend down in the proportion of opioid-related deaths occurring shortly after release from prison continued into 2014, when the figure was 3.1%, having steadily decreased since the start of the national naloxone programme.
chart. Also reduced was the combined total of post-prison and post-hospital deaths as a proportion of the total. Routinely collected statistics indicated that the trend down in the proportion of opioid-related deaths occurring shortly after release from prison continued into 2014, when the figure was 3.1%, having steadily decreased since the start of the national naloxone programme.
However, trends in deaths after release from hospital gave no corresponding indication that the programme had helped. Together with the increase in total opioid-related deaths in 2014 and 2015, it calls into question whether overall the programme has had the desired effects, even if it further reduced the small minority of deaths which occur after release from prison. Arguably, the national programme was underpowered. During the years of the evaluation, it supplied only about half the naloxone kits calculated as the target (8,000 a year) for a kit to be available at every witnessed opiate overdose.
Wales
Wales’s national naloxone programme began in 2011 after an evaluation of pilot schemes. These involved a single training session lasting one to two hours during which drug users (and in a few cases their friends and family) were trained to recognise the signs of overdose and how to respond with first aid and by administering naloxone, after which they were given a naloxone kit. Since its piloting in 2009 and up the end of 2015/16, 10,552 naloxone kits had been issued to 4,851 people, and 6,154 individuals had been trained in the administration of naloxone and overdose prevention.
The programme has been gathering pace. The number of individuals newly supplied kits rose 24% to 1058 in 2015/16 and the number of kits issued either as first-time supply or as a replacement rose 14% to 3,186. It has been calculated that for Wales the target for a kit to be available at every witnessed opiate overdose is 1700 kits a year. From data gathered at the time of resupply, kits were known to have been use 1,065 times, and more will have been used without the carrier returning for another kit. Of the 1,065 known uses, just 11 or about 1% were reported to have ended in a fatality. During 2015/16 a kit was known to have been used in the attempt to save life at least once for every nine individuals registered as carriers.
The programme has been linked to the decrease in drug misuse deaths in Wales, down by 17% from 162 in 2010 to 135 in both 2012 and 2013, but whether Wales’s programme really had affected the death rate was unclear. Even in the absence of a national naloxone programme, from 2010 to 2012 drug misuse deaths also fell (by 14%) in England. There they then rose steeply in 2013 to exceed the 2010 total while Wales sustained its reduction, seen in an article titled “Bucking the trend” as a vindication of Wales’s relative emphasis on harm reduction and de-emphasis on abstinence.
But the apparent success was to prove short-lived. The evidence had been a reduction in deaths registered in Wales in 2014 compared to a rise in England, but in fact that year there had also been a rise in Wales – in the number of deaths which actually occurred during the year. The following year these fed through to registered deaths to generate a sharp increase in 2015, a reversal which puzzled Public Health Wales.
Despite what may have turned out to be blip in the statistics, for its population of problem drug users and of problem opioid users in particular, Wales’ death rates in 2015 were still lower than in England and Scotland. Authorities there remain convinced that the naloxone programme is saving lives – “the single most effective intervention in the prevention of drug related deaths”.
Northern Ireland
In 2012 distribution of naloxone kits and associated training were piloted in Northern Ireland. Having planned to sample 40, evaluators were able to interview only 18 of the 362 opioid users at risk of overdose who by the end of August 2014 had been supplied a kit. Most did not carry their kits with them because they were no longer in drug using circles, or were concerned about stigma, harassment or legal/social consequences if found with naloxone on their person. Distribution primarily through treatment services both limited access and tended to confine it to opioid users in treatment.
Supported by the country’s Public Health Agency, the Council for the Homeless Northern Ireland now offers naloxone training to homelessness, pharmacy, and addictions services across Northern Ireland – “the first country globally to supply Naloxone to those at risk of overdose on a countrywide basis”.
Naloxone programmes face inherent limitations
Even if naloxone programmes work as hoped, they will always be only a partial solution to opioid overdose. They help prevent overdoses becoming fatal, while other interventions such as treatment and transitioning injectors to less dangerous routes of administration help prevent overdoses happening in the first place. In a context where having a naloxone kit may be seen as marking one out as an active drug user and offender, naloxone programmes are hampered by inherent limitations on the preparedness of people to be trained and to carry the kits. They can only be used if they are available at the right time and place, and if someone there is willing and able to use them ![]()
![]()
![]() more ...
more ...
Experts convened by the World Health Organization judged the “risk-benefit profile to be strongly in favour of naloxone distribution, due to its clear potential for saving lives and apparent low risk of significant adverse effects”, and strongly recommended naloxone provision and associated training for people likely to witness an opioid overdose. However, they also cautioned that this “does not address the underlying causes of opioid overdose”; further reducing the number of deaths would also entail monitoring and curbing inappropriate opioid prescribing and over-the-counter sales, and extending treatment for opioid dependence. Wider initiatives of this kind were among those recommended by Public Health England in its guidelines on preventing drug-related deaths and by the US authorities in their Opioid overdose toolkit.
Using alone
One of the limitations of naloxone is that if deaths occur among isolated people in their own homes, there is no one but the overdoser themselves to administer naloxone – something they may be unable to do. Even if it has been issued to the drug user concerned, this scenario (1 2) takes naloxone out of the equation and accounts for a high proportion of deaths. In Scotland in 2014, where this information was available only in 28% of incidents leading to a drug-related death was there another person in the room. Such figures are expected because if the drug users were not alone, they would have been less likely to die. Of more relevance is the proportion of opioid uses which occur when the user is alone, making naloxone less likely to be administered. In England for example, after release from prison about half the heroin users who returned survey forms indicating that they had injected in the first two weeks also said they had done so alone, and on average they had injected alone two-thirds of the time.
Issued but not available
Outside their homes, unless they are carrying naloxone with them, drug users issued the kits will not be in a position to use them or have them used by others. In Northern Ireland not having the kit with you was one of the reasons why it was not used in actual overdose incidents. In Scotland too, reluctance to carry the kits around may have undermined the programme’s potential to save lives. Though some trainees kept their kits with them all the time, others left it at home due to concerns that it would expose them as a drug user if seen by the police, leading to detention and search and targeting in future. A survey of needle exchange attendees in Scotland found that among the minority who had injected in the past but not in the last six months, very few carried the kits they had been given – in 2011–2012 just 5%, and in 2013–2014, just 1%, the latter figure representing one person out of 81. But even among more recent injectors, in 2013–2014 just 6% were carrying a kit when interviewed.
A trial in England of prison-release naloxone packaged the pre-filled syringe and related information in a special wallet which also functions as a regular wallet – unobtrusive, multi-use packaging which users may be more likely to take with them than a boxed naloxone kit. Of 112 prisoners who completed follow-up surveys when reimprisoned within six months, 71% said that in the first two weeks after release they had carried the naloxone kit around with them, perhaps corresponding to the 69% who had returned to heroin use during that period. Another 654 (ex-)prisoners had not returned survey forms. How many also carried the drug around with them is unknown, as is whether carriage was maintained beyond the first two weeks, but the results that are known suggest high carriage rates can be engineered.
In Scotland in 2014, of the 34 cases where it was known that the deceased had been issued a naloxone kit and also known whether it was available at the time of death, the kit was used to try to save them in just 9 cases. Generally this was because only in 13 of the incidents was the naloxone available at the time, while in others it was available but there was no other person around to administer it. These figures show deaths can and do happen due to non-availability of issued kits, though many other deaths may have been prevented by the kits being available.
Though universal carriage may be the ideal, in England in 2013 around 70% of drug-related deaths occurred in the person’s home or at another private residential address, such as a friend’s home. In Scotland in 2014, two-thirds of the people who died a drug-related death had taken their drugs (67%) and died (63%) in their own homes. In these circumstances, a naloxone kit may be present even if not carried about in pockets or handbags.
If still aware enough, the person at risk may themselves refuse naloxone (1 2) for fear of it precipitating withdrawal or because the effect of their expensive dose of heroin will be nullified.
When it is administered, naloxone does not always prevent deaths. In Scotland in 2014, of 21 deaths involving opioids where naloxone was known to be available, it was administered in 18 cases. Why this failed to prevent the deaths is not known.
Another limitation is that for treatment services – especially those with a recovery orientation – catering for the likelihood that their patients will not recover but relapse to life-threatening opiate use may be a hard pill to swallow; swallowing it by training clients and families to prepare for relapse may seem to counter-therapeutically undermine the optimism at the heart of the recovery movement. Similarly, for patients looking forward to a new life where they have escaped drugs and drugtaking circles, learning a lifesaving technique predicated on continued contact with (largely) injecting drug use(rs) can seem undermining and irrelevant.
More information
For more on the promise and limitations of naloxone see this analysis of a British study of a naloxone training programme. Further guidance is available in the appendices to a study conducted by the English National Treatment Agency for Substance Misuse. In 2008 staff from one of the English NHS trusts which piloted naloxone training for families and carers produced a UK-focused practical guide to naloxone prescribing, training and use. The Scottish Drugs Forum runs a web site offering naloxone-related resources, advice, guidance, information and news. The organisation for GPs in Britain with an interest in managing substance use problems runs a free online course on using naloxone to prevent overdose. Under the banner of the Open Society Foundation, an international collaboration has come together to offer advice and practical assistance on starting a take-home naloxone programme. European Union guidance and information on naloxone includes advice on setting up take-home naloxone training and distribution programmes, and a European group of experts on drug-related deaths and their prevention has contributed wide-ranging policy and practice advice on opioid overdose. Guidance on overdose prevention in general with an emphasis on the role of naloxone has also been produced by the Eurasian Harm Reduction Network. In the USA the Chicago Recovery Alliance has produced a freely available training video. A video on responding to an overdose and administering naloxone has also been made freely available by the study in England of prison-release naloxone. The manufacturers of the naloxone preparation Prenoxad also offer advice on its use.
The many contributors to overdoses and possible strategies to prevent them were reviewed by Findings in a two-part series and in another hot topic. Drug consumption rooms are another way to prevent overdose deaths, the evidence for which and UK policy were the subject of another hot topic. A further hot topic has discussed the concept of harm reduction in general.
Thanks for their comments on this entry in draft to Sheila Bird of the University of Cambridge in England. Commentators bear no responsibility for the text including the interpretations and any remaining errors.
Last revised 24 April 2017. First uploaded 10 February 2017
![]() Comment/query
Comment/query![]() Open Effectiveness Bank home page
Open Effectiveness Bank home page
Top 10 most closely related documents on this site. For more try a subject or free text search
HOT TOPIC 2017 Overdose deaths in the UK: crisis and response
DOCUMENT 2014 Community management of opioid overdose
STUDY 2011 The NTA overdose and naloxone training programme for families and carers
DOCUMENT 2017 Drug misuse and dependence: UK guidelines on clinical management
MATRIX CELL 2017 Drug Matrix cell C1: Management/supervision: Reducing harm